People with diabetes face a high risk of foot complications. Adding podiatrists to their care team helps reduce these risks.
Diabetic neuropathy causes numbness and tingling in the feet, and reduced blood flow means that cuts and sores may not be noticed. This can lead to serious infections that can’t heal.
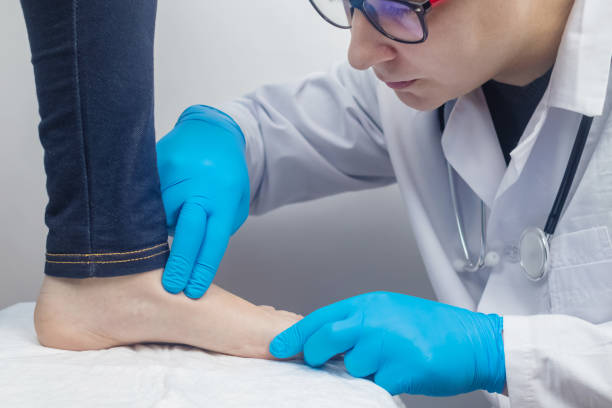
Prevention
Diabetes and foot problems go hand in hand, and if left unchecked, can lead to severe complications, including lower extremity amputation. Podiatrist High Wycombe conduct thorough foot examinations and identify potential abnormalities, like calluses, blisters or ingrown toenails, which could be symptoms of nerve damage (neuropathy). They are also experts in diabetic wound care and can recommend specialized footwear to help redistribute pressure and prevent ulcers from developing.
High levels of blood glucose can cause poor circulation in the feet and legs, hampering nutrient flow and sensation. This is known as peripheral neuropathy and can affect a person’s ability to feel pain, making them more susceptible to injury and infection. They are skilled in identifying early signs of neuropathy by conducting tests like monofilament and tuning fork testing, which can detect any changes in sensitivity or reflexes.
They can also help reduce the risk of developing foot complications by educating patients on good daily foot care practices, encouraging them to regularly inspect their feet and keeping them clean and dry. They can also provide splinting, padding and custom orthotics to reduce excessive foot strain. In addition, They are trained to recognize the difference between a simple foot ulcer and a serious one and can use advanced techniques to treat infections and promote healthy tissue growth. They are also experienced in implementing multidisciplinary diabetic foot limb salvage programs.
Treatment
Diabetic neuropathy can affect the nerves in your feet and legs, causing tingling or numbness. This makes it harder to tell when you have a cut or sore in your foot, which can lead to serious infections. A podiatrist can help manage your symptoms and keep you safe by assessing your blood flow to your feet. This can be done with a test similar to your blood pressure, where the podiatrist puts pressure on the tip of your big toe and then in each shoe to establish how much blood is flowing to the foot.
A podiatry based in Midland can treat common foot problems that arise with diabetes, including corns, calluses, hammertoes, ingrown toenails, bunions, heel spurs, and shortened or weakened tendons and ligaments. They can also use cryotherapy equipment to freeze off plantar warts. They can prescribe specialized footwear and orthotics for flat feet, as well as braces to support weak or injured foot ligaments.
The best way to prevent complications from diabetes is to get your blood sugar under control. Adding a podiatrist to your healthcare team is the next step. Make sure you are getting your foot checks at every health care visit and that you know how to check your feet for signs of problems. This can save you from amputation, as 70% of lower limb amputations in Americans are the result of diabetic foot problems.

Early Detection
A good way to prevent diabetes-related foot problems is to see a podiatrist regularly. During an exam, your podiatrist will assess the condition of your feet and ankles and look for signs of common diabetic foot issues. They can also help you keep track of your blood sugar levels and recommend ways to prevent or treat complications associated with diabetes.
Diabetics can experience a variety of foot issues that can cause significant damage to the feet and legs. These problems include nerve damage (neuropathy) and reduced circulation to the feet (peripheral arterial disease). Nerve damage can reduce sensation in the feet, making it harder for you to notice a wound or other injury. Poor circulation can slow down the body’s ability to heal injuries and increase your risk for severe infections.
Podiatrists can detect early signs of diabetic foot conditions by performing a simple assessment, called a toe pressure test. This test is similar to taking your blood pressure and measures the amount of blood flow reaching the toes.
In addition, your podiatrist can teach you how to do daily foot exams and help you select appropriate footwear to protect your feet from injuries. They can also provide advice on non-surgical treatments like splinting, padding and custom orthotics to alleviate symptoms and improve foot function.
Education
Diabetes requires diligent blood sugar control and careful attention to the entire body, including the feet. Podiatrists help patients recognize the importance of daily foot inspections to catch potential problems before they worsen. They also provide detailed guidance on choosing specialized footwear that considers cushioning, breathability and arch support.
They help educate diabetics on foot care practices that prevent complications, such as keeping the feet clean and moisturized, avoiding cuts and abrasions, and proper footwear selection. They also explain how to check the feet for signs of swelling, redness or numbness. This is particularly important because diabetic neuropathy can cause a loss of sensation in the lower extremities, so people may not feel an injury or complication in the foot until it is too late.
In addition, podiatrists are experts in wound care and infection management for the diabetic foot. They are able to recognize when an ingrown toenail or paronychia (a soft swelling around the base of the toe nail) has progressed to ascending cellulitis or osteomyelitis, and provide aggressive treatment (broad-spectrum antibiotics, radiographs to exclude osteomyelitis and close monitoring) that may save the limb. They can also provide non-surgical interventions like splinting and padding and recommend custom orthotics to alleviate symptoms or improve foot function. This helps reduce the risk of serious lower leg and foot deformities, such as hammertoes and bunions, which can lead to pain and difficulty with walking.




